Main Article Content
Abstract
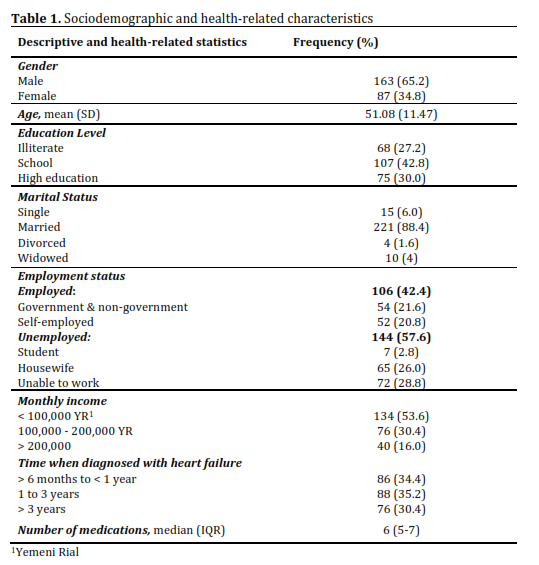
Beliefs about medication influence treatment engagement and outcomes in patients with heart failure, yet evidence from low-resource settings such as Yemen remains limited due to under-supported health care systems and low monitoring in health services. To assess medication beliefs among heart failure patients in Yemen and examine factors associated with necessity and concern beliefs, including medication regimen complexity. A hospital-based cross-sectional study was conducted between December 2023 and February 2024 among heart failure patients attending cardiology outpatient clinics in Sana’a, Yemen after ethical approval from the hospital. Data were collected using structured questionnaires, including the Beliefs About Medication Questionnaire (BMQ-Specific) and the Medication Regimen Complexity Index (MRCI). Multivariable linear regression analyses were performed to identify predictors of medication beliefs. A total of 250 patients were included, with a mean age of 51.08±11.47 years, and 65.2% were male. The median total BMQ score was 38.0 (IQR:35–42). Higher necessity beliefs were independently associated with older age (B=0.046, p=0.029), higher educational status (B=−1.240, p=0.030), and a greater number of prescribed medications (B=0.802, p=0.001), whereas greater medication regimen complexity was negatively associated with necessity beliefs (B=−0.276, p=0.003). Regarding concern beliefs, employment status (B=2.605, p<0.001) and longer duration since diagnosis (>3 years) (B=−1.155, p=0.029) were significant predictors, indicating a mild but significant impact. No significant associations were observed between concern beliefs and age, gender, education, income, number of medications, or regimen complexity. Medication beliefs among heart failure patients in Yemen are shaped by both patient and treatment-related factors. The findings have important implications in clinical practice, both clinical pharmacists and cardiologist can consider patients’ perspective to guide intervention design especially simplifying medication regimens and addressing patient-specific concerns.
Article Details

This work is licensed under a Creative Commons Attribution 4.0 International License.
References
- Abdelbary, A., Kaddoura, R., Balushi, S. A., Ahmed, S., Galvez, R., Ahmed, A., Nashwan, A. J., Alnaimi, S., Al Hail, M., & Elbdri, S. (2023). Implications of the medication regimen complexity index score on hospital readmissions in elderly patients with heart failure: A retrospective cohort study. BMC Geriatrics, 23(1), 377. https://doi.org/10.1186/s12877-023-04062-2
- Advinha, A. M., de Oliveira-Martins, S., Mateus, V., Pajote, S. G., & Lopes, M. J. (2014). Medication regimen complexity in institutionalized elderly people in an aging society. International Journal of Clinical Pharmacy, 36(4), 750–756. https://doi.org/10.1007/s11096-014-9963-4
- Aksoy, N., Ozturk, N., Okuyan, B., & Sancar, M. (2023). Validation of the Arabic Version of Medication Regimen Complexity Index Among Older Patients—Validation of the “MRCI-Arabic.” Sudan Journal of Medical Sciences, 18(3), Article 3.
- Alfaqeeh M, Abdullah R, Zakiyah N, Suwantika AA, Postma MJ, Rahmawati F, Widayanti AW, Ibrahim B. Medication Adherence and Contributing Factors in Patients with Heart Failure Within the Middle East: A Systematic Review. Glob Heart. 2025 May 27;20(1):47. doi: 10.5334/gh.1431. PMID: 40454105; PMCID: PMC12124249.
- AlGhurair, S. A., Hughes, C. A., Simpson, S. H., & Guirguis, L. M. (2012). A systematic review of patient self-reported barriers of adherence to antihypertensive medications using the world health organization multidimensional adherence model. Journal of Clinical Hypertension (Greenwich, Conn.), 14(12), 877–886. https://doi.org/10.1111/j.1751-7176.2012.00699.x
- Alhewiti, A. (2014). Adherence to Long-Term Therapies and Beliefs about Medications. International Journal of Family Medicine, 2014, 479596. https://doi.org/10.1155/2014/479596
- Al-Ruthia, Y. S., Hong, S. H., Graff, C., Kocak, M., Solomon, D., & Nolly, R. (2017). Examining the relationship between antihypertensive medication satisfaction and adherence in older patients. Research in Social & Administrative Pharmacy: RSAP, 13(3), 602–613. https://doi.org/10.1016/j.sapharm.2016.06.013
- Alsous, M., Alhalaiqa, F., Abu Farha, R., Abdel Jalil, M., McElnay, J., & Horne, R. (2017). Reliability and validity of Arabic translation of Medication Adherence Report Scale (MARS) and Beliefs about Medication Questionnaire (BMQ)-specific for use in children and their parents. PloS One, 12(2), e0171863. https://doi.org/10.1371/journal.pone.0171863
- Bai, H.-H., Nie, X.-J., Chen, X.-L., Liang, N.-J., Peng, L.-R., & Yao, Y.-Q. (2022). Beliefs about medication and their association with adherence in Chinese patients with non-dialysis chronic kidney disease stages 3-5. Medicine, 101(2), e28491. https://doi.org/10.1097/MD.0000000000028491
- Barry, A. R., Wang, E. H. Z., Chua, D., Zhou, L., Hong, K. M. H., Safari, A., & Loewen, P. (2023). Patients’ Beliefs About Their Cardiovascular Medications After Acute Coronary Syndrome: A Prospective Observational Study. CJC Open, 5(10), 745–753. https://doi.org/10.1016/j.cjco.2023.07.004
- Beezer, J., Al Hatrushi, M., Husband, A., Kurdi, A., & Forsyth, P. (2022). Polypharmacy definition and prevalence in heart failure: A systematic review. Heart Failure Reviews, 27(2), 465–492. https://doi.org/10.1007/s10741-021-10135-4
- Choudhry, N. K., Fischer, M. A., Avorn, J., Liberman, J. N., Schneeweiss, S., Pakes, J., Brennan, T. A., & Shrank, W. H. (2011). The implications of therapeutic complexity on adherence to cardiovascular medications. Archives of Internal Medicine, 171(9), 814–822. https://doi.org/10.1001/archinternmed.2010.495
- Claxton, A. J., Cramer, J., & Pierce, C. (2001). A systematic review of the associations between dose regimens and medication compliance. Clinical Therapeutics, 23(8), 1296–1310. https://doi.org/10.1016/S0149-2918(01)80109-0
- Clyne, B., Cooper, J. A., Boland, F., Hughes, C. M., Fahey, T., Smith, S. M., & OPTI-SCRIPT study team. (2017). Beliefs about prescribed medication among older patients with polypharmacy: A mixed methods study in primary care. The British Journal of General Practice: The Journal of the Royal College of General Practitioners, 67(660), e507–e518. https://doi.org/10.3399/bjgp17X691073
- Cobretti, M. R., Page, R. L., Linnebur, S. A., Deininger, K. M., Ambardekar, A. V., Lindenfeld, J., & Aquilante, C. L. (2017). Medication regimen complexity in ambulatory older adults with heart failure. Clinical Interventions in Aging, 12, 679–686. https://doi.org/10.2147/CIA.S130832
- Dias, A., Pereira, C., Monteiro, M. J., & Santos, C. (2014). Patients’ beliefs about medicines and adherence to medication in ischemic heart disease. Atención Primaria, 46, 101–106. https://doi.org/10.1016/S0212-6567(14)70074-5
- Emilsson, M., Berndtsson, I., Gustafsson, P. A., Horne, R., & Marteinsdottir, I. (2020). Reliability and validation of Swedish translation of Beliefs about Medication Specific (BMQ-Specific) and Brief Illness Perception Questionnaire (B-IPQ) for use in adolescents with attention-deficit hyperactivity disorder. Nordic Journal of Psychiatry, 74(2), 89–95. https://doi.org/10.1080/08039488.2019.1674376
- Farrell B, French Merkley V, Ingar N. Reducing pill burden and helping with medication awareness to improve adherence. Can Pharm J (Ott). 2013 Sep;146(5):262-9. doi: 10.1177/1715163513500208. PMID: 24093037; PMCID: PMC3785195.
- Ferreira, J. M., Galato, D., & Melo, A. C. (2015). Medication regimen complexity in adults and the elderly in a primary healthcare setting: Determination of high and low complexities. Pharmacy Practice, 13(4), 659. https://doi.org/10.18549/PharmPract.2015.04.659
- Fröhlich, S. E., Zaccolo, A. V., da Silva, S. L. C., & Mengue, S. S. (2010). Association between drug prescribing and quality of life in primary care. Pharmacy World & Science: PWS, 32(6), 744–751. https://doi.org/10.1007/s11096-010-9431-8
- Fuller, J. M., Barenfeld, E., & Ekman, I. (2021). Why do patients struggle with their medicines?-A phenomenological hermeneutical study of how patients experience medicines in their everyday lives. PloS one, 16(8), e0255478. https://doi.org/10.1371/journal.pone.0255478
- Gatti, M. E., Jacobson, K. L., Gazmararian, J. A., Schmotzer, B., & Kripalani, S. (2009). Relationships between beliefs about medications and adherence. American Journal of Health-System Pharmacy: AJHP: Official Journal of the American Society of Health-System Pharmacists, 66(7), 657–664. https://doi.org/10.2146/ajhp080064
- George, J., Phun, Y.-T., Bailey, M. J., Kong, D. C. M., & Stewart, K. (2004). Development and validation of the medication regimen complexity index. The Annals of Pharmacotherapy, 38(9), 1369–1376. https://doi.org/10.1345/aph.1D479
- Hajjar, E. R., Cafiero, A. C., & Hanlon, J. T. (2007). Polypharmacy in elderly patients. The American Journal of Geriatric Pharmacotherapy, 5(4), 345–351. https://doi.org/10.1016/j.amjopharm.2007.12.002
- Hassan, M. (2015). Gulf CARE: Heart failure in the Middle East. Global Cardiology Science & Practice, 2015(3), 34. https://doi.org/10.5339/gcsp.2015.34
- Hirsch, J. D., Metz, K. R., Hosokawa, P. W., & Libby, A. M. (2014). Validation of a patient-level medication regimen complexity index as a possible tool to identify patients for medication therapy management intervention. Pharmacotherapy, 34(8), 826–835. https://doi.org/10.1002/phar.1452
- Horne, R., Weinman, J., & Hankins, M. (1999). The beliefs about medicines questionnaire: The development and evaluation of a new method for assessing the cognitive representation of medication. Psychology & Health, 14(1), 1–24. https://doi.org/10.1080/08870449908407311
- Ingersoll, K. S., & Cohen, J. (2008). The impact of medication regimen factors on adherence to chronic treatment: A review of literature. Journal of Behavioral Medicine, 31(3), 213–224. https://doi.org/10.1007/s10865-007-9147-y
- Jiang, S., Zhu, Z., Liao, G., Huang, Y., Li, L., & Zeng, K. (2023). Relationship Between Medication Literacy and Beliefs Among Persons with Type 2 Diabetes Mellitus in Guangdong, China. Patient Preference and Adherence, 17, 2039–2050. https://doi.org/10.2147/PPA.S420383
- Kassaw, A. T., Sendekie, A. K., Minyihun, A., & Gebresillassie, B. M. (2024). Medication regimen complexity and its impact on medication adherence in patients with multimorbidity at a comprehensive specialized hospital in Ethiopia. Frontiers in Medicine, 11. https://doi.org/10.3389/fmed.2024.1369569
- Khan, M. S., Shahid, I., Fonarow, G. C., & Greene, S. J. (2022). Classifying heart failure based on ejection fraction: Imperfect but enduring. European Journal of Heart Failure, 24(7), 1154–1157. https://doi.org/10.1002/ejhf.2470
- Laradhi AO, Shan Y, Mansoor Al Raimi A, Hussien NA, Ragab E, Getu MA, Al-Bani G, Allawy ME. The association of illness perception and related factors with treatment adherence among chronic hemodialysis patients with cardio-renal syndrome in Yemen. Front Cardiovasc Med. 2025 Apr 30;12:1432648. doi: 10.3389/fcvm.2025.1432648. PMID: 40371064; PMCID: PMC12075227.
- Lee SY, Lee S, Lee W. Association between medication adherence to chronic diseases and shift-work schedules in the Korean working population. Sci Rep. 2022 Dec 30;12(1):22595. doi: 10.1038/s41598-022-26618-9. PMID: 36585432; PMCID: PMC9803658.
- Li, R. (2024). Association between Psychological Distress, Employment Status and Medication Adherence among Adult Hypertensive Patient. Theoretical and Natural Science, 64, 50–56. https://doi.org/10.54254/2753-8818/64/20241666
- Lund, L. H., Pitt, B., & Metra, M. (2022). Left ventricular ejection fraction as the primary heart failure phenotyping parameter. European Journal of Heart Failure, 24(7), 1158–1161. https://doi.org/10.1002/ejhf.2576
- Ma, X., Jung, C., Chang, H.-Y., Richards, T. M., & Kharrazi, H. (2020). Assessing the Population-Level Correlation of Medication Regimen Complexity and Adherence Indices Using Electronic Health Records and Insurance Claims. Journal of Managed Care & Specialty Pharmacy, 26(7), 10.18553/jmcp.2020.26.7.860. https://doi.org/10.18553/jmcp.2020.26.7.860
- Mansur, N., Weiss, A., & Beloosesky, Y. (2012). Looking beyond polypharmacy: Quantification of medication regimen complexity in the elderly. The American Journal of Geriatric Pharmacotherapy, 10(4), 223–229. https://doi.org/10.1016/j.amjopharm.2012.06.002
- Masoudi, F. A., & Krumholz, H. M. (2003). Polypharmacy and comorbidity in heart failure. BMJ : British Medical Journal, 327(7414), 513–514.
- Mastromarino, V., Casenghi, M., Testa, M., Gabriele, E., Coluccia, R., Rubattu, S., & Volpe, M. (2014). Polypharmacy in heart failure patients. Current Heart Failure Reports, 11(2), 212–219. https://doi.org/10.1007/s11897-014-0186-8
- Pantuzza, L. L., Ceccato, M. das G. B., Silveira, M. R., Junqueira, L. M. R., & Reis, A. M. M. (2017). Association between medication regimen complexity and pharmacotherapy adherence: A systematic review. European Journal of Clinical Pharmacology, 73(11), 1475–1489. https://doi.org/10.1007/s00228-017-2315-2
- Percival, M., Cottrell, W. N., & Jayasinghe, R. (2012). Exploring the beliefs of heart failure patients towards their heart failure medicines and self care activities. International Journal of Clinical Pharmacy, 34(4), 618–625. https://doi.org/10.1007/s11096-012-9655-x
- Phillips, L. A., Diefenbach, M., Kronish, I. M., Negron, R. M., & Horowitz, C. R. (2014). The Necessity-Concerns-Framework: A Multidimensional Theory Benefits from Multidimensional Analysis. Annals of Behavioral Medicine : A Publication of the Society of Behavioral Medicine, 48(1), 7–16. https://doi.org/10.1007/s12160-013-9579-2
- Rafhi, E., Stupans, I., Stevens, J. E., Soo Park, J., & Wang, K. N. (2025). The influence of beliefs and health literacy on medication-related outcomes in older adults: A cross-sectional study. Research in Social and Administrative Pharmacy, 21(1), 47–55. https://doi.org/10.1016/j.sapharm.2024.10.003
- Safwana Al-Tahesh et al. Predictors and impact of medication non-adherence in heart failure patients: a retrospective cohort from a tertiary hospital in Yemen. Pan African Medical Journal. 2026;53:9. [doi: 10.11604/pamj.2026.53.9.48712]
- Savarese, G., Stolfo, D., Sinagra, G., & Lund, L. H. (2022). Heart failure with mid-range or mildly reduced ejection fraction. Nature Reviews. Cardiology, 19(2), 100–116. https://doi.org/10.1038/s41569-021-00605-5
- Schoonover, H., Corbett, C. F., Weeks, D. L., Willson, M. N., & Setter, S. M. (2014). Predicting potential postdischarge adverse drug events and 30-day unplanned hospital readmissions from medication regimen complexity. Journal of Patient Safety, 10(4), 186–191. https://doi.org/10.1097/PTS.0000000000000067
- Stange, D., Kriston, L., von Wolff, A., Baehr, M., & Dartsch, D. C. (2013). Medication complexity, prescription behaviour and patient adherence at the interface between ambulatory and stationary medical care. European Journal of Clinical Pharmacology, 69(3), 573–580. https://doi.org/10.1007/s00228-012-1342-2
- Supramaniam, P., binti Ali, A., Li Yun, C., Pei Yi, C., binti Shaari, A., binti Kamaruzaman, N. H., Jia Yi, S., Keat Ming, T., Yuan Liang, W., & Pei Wen, Y. (2019). Reliability and validity of Beliefs on Medicine Questionnaire (BMQ) in diabetes mellitus patients: Malay Translated Version. International Journal of Scientific and Research Publications (IJSRP), 9(2), p8609. https://doi.org/10.29322/IJSRP.9.02.2019.p8609
- Wei, L., Champman, S., Li, X., Li, X., Li, S., Chen, R., Bo, N., Chater, A., & Horne, R. (2017). Beliefs about medicines and non-adherence in patients with stroke, diabetes mellitus and rheumatoid arthritis: A cross-sectional study in China. BMJ Open, 7(10), e017293. https://doi.org/10.1136/bmjopen-2017-017293
- Yasin, N. M., Filliana, U., & Kristina, S. A. (2024). Pengaruh Brief Counseling Apoteker terhadap Kepatuhan Pengobatan dan Perbaikan Tekanan Darah Pasien Hemodialisa. Majalah Farmaseutik, 20(3), 324. https://doi.org/10.22146/FARMASEUTIK.V20I3.92562.
References
Abdelbary, A., Kaddoura, R., Balushi, S. A., Ahmed, S., Galvez, R., Ahmed, A., Nashwan, A. J., Alnaimi, S., Al Hail, M., & Elbdri, S. (2023). Implications of the medication regimen complexity index score on hospital readmissions in elderly patients with heart failure: A retrospective cohort study. BMC Geriatrics, 23(1), 377. https://doi.org/10.1186/s12877-023-04062-2
Advinha, A. M., de Oliveira-Martins, S., Mateus, V., Pajote, S. G., & Lopes, M. J. (2014). Medication regimen complexity in institutionalized elderly people in an aging society. International Journal of Clinical Pharmacy, 36(4), 750–756. https://doi.org/10.1007/s11096-014-9963-4
Aksoy, N., Ozturk, N., Okuyan, B., & Sancar, M. (2023). Validation of the Arabic Version of Medication Regimen Complexity Index Among Older Patients—Validation of the “MRCI-Arabic.” Sudan Journal of Medical Sciences, 18(3), Article 3.
Alfaqeeh M, Abdullah R, Zakiyah N, Suwantika AA, Postma MJ, Rahmawati F, Widayanti AW, Ibrahim B. Medication Adherence and Contributing Factors in Patients with Heart Failure Within the Middle East: A Systematic Review. Glob Heart. 2025 May 27;20(1):47. doi: 10.5334/gh.1431. PMID: 40454105; PMCID: PMC12124249.
AlGhurair, S. A., Hughes, C. A., Simpson, S. H., & Guirguis, L. M. (2012). A systematic review of patient self-reported barriers of adherence to antihypertensive medications using the world health organization multidimensional adherence model. Journal of Clinical Hypertension (Greenwich, Conn.), 14(12), 877–886. https://doi.org/10.1111/j.1751-7176.2012.00699.x
Alhewiti, A. (2014). Adherence to Long-Term Therapies and Beliefs about Medications. International Journal of Family Medicine, 2014, 479596. https://doi.org/10.1155/2014/479596
Al-Ruthia, Y. S., Hong, S. H., Graff, C., Kocak, M., Solomon, D., & Nolly, R. (2017). Examining the relationship between antihypertensive medication satisfaction and adherence in older patients. Research in Social & Administrative Pharmacy: RSAP, 13(3), 602–613. https://doi.org/10.1016/j.sapharm.2016.06.013
Alsous, M., Alhalaiqa, F., Abu Farha, R., Abdel Jalil, M., McElnay, J., & Horne, R. (2017). Reliability and validity of Arabic translation of Medication Adherence Report Scale (MARS) and Beliefs about Medication Questionnaire (BMQ)-specific for use in children and their parents. PloS One, 12(2), e0171863. https://doi.org/10.1371/journal.pone.0171863
Bai, H.-H., Nie, X.-J., Chen, X.-L., Liang, N.-J., Peng, L.-R., & Yao, Y.-Q. (2022). Beliefs about medication and their association with adherence in Chinese patients with non-dialysis chronic kidney disease stages 3-5. Medicine, 101(2), e28491. https://doi.org/10.1097/MD.0000000000028491
Barry, A. R., Wang, E. H. Z., Chua, D., Zhou, L., Hong, K. M. H., Safari, A., & Loewen, P. (2023). Patients’ Beliefs About Their Cardiovascular Medications After Acute Coronary Syndrome: A Prospective Observational Study. CJC Open, 5(10), 745–753. https://doi.org/10.1016/j.cjco.2023.07.004
Beezer, J., Al Hatrushi, M., Husband, A., Kurdi, A., & Forsyth, P. (2022). Polypharmacy definition and prevalence in heart failure: A systematic review. Heart Failure Reviews, 27(2), 465–492. https://doi.org/10.1007/s10741-021-10135-4
Choudhry, N. K., Fischer, M. A., Avorn, J., Liberman, J. N., Schneeweiss, S., Pakes, J., Brennan, T. A., & Shrank, W. H. (2011). The implications of therapeutic complexity on adherence to cardiovascular medications. Archives of Internal Medicine, 171(9), 814–822. https://doi.org/10.1001/archinternmed.2010.495
Claxton, A. J., Cramer, J., & Pierce, C. (2001). A systematic review of the associations between dose regimens and medication compliance. Clinical Therapeutics, 23(8), 1296–1310. https://doi.org/10.1016/S0149-2918(01)80109-0
Clyne, B., Cooper, J. A., Boland, F., Hughes, C. M., Fahey, T., Smith, S. M., & OPTI-SCRIPT study team. (2017). Beliefs about prescribed medication among older patients with polypharmacy: A mixed methods study in primary care. The British Journal of General Practice: The Journal of the Royal College of General Practitioners, 67(660), e507–e518. https://doi.org/10.3399/bjgp17X691073
Cobretti, M. R., Page, R. L., Linnebur, S. A., Deininger, K. M., Ambardekar, A. V., Lindenfeld, J., & Aquilante, C. L. (2017). Medication regimen complexity in ambulatory older adults with heart failure. Clinical Interventions in Aging, 12, 679–686. https://doi.org/10.2147/CIA.S130832
Dias, A., Pereira, C., Monteiro, M. J., & Santos, C. (2014). Patients’ beliefs about medicines and adherence to medication in ischemic heart disease. Atención Primaria, 46, 101–106. https://doi.org/10.1016/S0212-6567(14)70074-5
Emilsson, M., Berndtsson, I., Gustafsson, P. A., Horne, R., & Marteinsdottir, I. (2020). Reliability and validation of Swedish translation of Beliefs about Medication Specific (BMQ-Specific) and Brief Illness Perception Questionnaire (B-IPQ) for use in adolescents with attention-deficit hyperactivity disorder. Nordic Journal of Psychiatry, 74(2), 89–95. https://doi.org/10.1080/08039488.2019.1674376
Farrell B, French Merkley V, Ingar N. Reducing pill burden and helping with medication awareness to improve adherence. Can Pharm J (Ott). 2013 Sep;146(5):262-9. doi: 10.1177/1715163513500208. PMID: 24093037; PMCID: PMC3785195.
Ferreira, J. M., Galato, D., & Melo, A. C. (2015). Medication regimen complexity in adults and the elderly in a primary healthcare setting: Determination of high and low complexities. Pharmacy Practice, 13(4), 659. https://doi.org/10.18549/PharmPract.2015.04.659
Fröhlich, S. E., Zaccolo, A. V., da Silva, S. L. C., & Mengue, S. S. (2010). Association between drug prescribing and quality of life in primary care. Pharmacy World & Science: PWS, 32(6), 744–751. https://doi.org/10.1007/s11096-010-9431-8
Fuller, J. M., Barenfeld, E., & Ekman, I. (2021). Why do patients struggle with their medicines?-A phenomenological hermeneutical study of how patients experience medicines in their everyday lives. PloS one, 16(8), e0255478. https://doi.org/10.1371/journal.pone.0255478
Gatti, M. E., Jacobson, K. L., Gazmararian, J. A., Schmotzer, B., & Kripalani, S. (2009). Relationships between beliefs about medications and adherence. American Journal of Health-System Pharmacy: AJHP: Official Journal of the American Society of Health-System Pharmacists, 66(7), 657–664. https://doi.org/10.2146/ajhp080064
George, J., Phun, Y.-T., Bailey, M. J., Kong, D. C. M., & Stewart, K. (2004). Development and validation of the medication regimen complexity index. The Annals of Pharmacotherapy, 38(9), 1369–1376. https://doi.org/10.1345/aph.1D479
Hajjar, E. R., Cafiero, A. C., & Hanlon, J. T. (2007). Polypharmacy in elderly patients. The American Journal of Geriatric Pharmacotherapy, 5(4), 345–351. https://doi.org/10.1016/j.amjopharm.2007.12.002
Hassan, M. (2015). Gulf CARE: Heart failure in the Middle East. Global Cardiology Science & Practice, 2015(3), 34. https://doi.org/10.5339/gcsp.2015.34
Hirsch, J. D., Metz, K. R., Hosokawa, P. W., & Libby, A. M. (2014). Validation of a patient-level medication regimen complexity index as a possible tool to identify patients for medication therapy management intervention. Pharmacotherapy, 34(8), 826–835. https://doi.org/10.1002/phar.1452
Horne, R., Weinman, J., & Hankins, M. (1999). The beliefs about medicines questionnaire: The development and evaluation of a new method for assessing the cognitive representation of medication. Psychology & Health, 14(1), 1–24. https://doi.org/10.1080/08870449908407311
Ingersoll, K. S., & Cohen, J. (2008). The impact of medication regimen factors on adherence to chronic treatment: A review of literature. Journal of Behavioral Medicine, 31(3), 213–224. https://doi.org/10.1007/s10865-007-9147-y
Jiang, S., Zhu, Z., Liao, G., Huang, Y., Li, L., & Zeng, K. (2023). Relationship Between Medication Literacy and Beliefs Among Persons with Type 2 Diabetes Mellitus in Guangdong, China. Patient Preference and Adherence, 17, 2039–2050. https://doi.org/10.2147/PPA.S420383
Kassaw, A. T., Sendekie, A. K., Minyihun, A., & Gebresillassie, B. M. (2024). Medication regimen complexity and its impact on medication adherence in patients with multimorbidity at a comprehensive specialized hospital in Ethiopia. Frontiers in Medicine, 11. https://doi.org/10.3389/fmed.2024.1369569
Khan, M. S., Shahid, I., Fonarow, G. C., & Greene, S. J. (2022). Classifying heart failure based on ejection fraction: Imperfect but enduring. European Journal of Heart Failure, 24(7), 1154–1157. https://doi.org/10.1002/ejhf.2470
Laradhi AO, Shan Y, Mansoor Al Raimi A, Hussien NA, Ragab E, Getu MA, Al-Bani G, Allawy ME. The association of illness perception and related factors with treatment adherence among chronic hemodialysis patients with cardio-renal syndrome in Yemen. Front Cardiovasc Med. 2025 Apr 30;12:1432648. doi: 10.3389/fcvm.2025.1432648. PMID: 40371064; PMCID: PMC12075227.
Lee SY, Lee S, Lee W. Association between medication adherence to chronic diseases and shift-work schedules in the Korean working population. Sci Rep. 2022 Dec 30;12(1):22595. doi: 10.1038/s41598-022-26618-9. PMID: 36585432; PMCID: PMC9803658.
Li, R. (2024). Association between Psychological Distress, Employment Status and Medication Adherence among Adult Hypertensive Patient. Theoretical and Natural Science, 64, 50–56. https://doi.org/10.54254/2753-8818/64/20241666
Lund, L. H., Pitt, B., & Metra, M. (2022). Left ventricular ejection fraction as the primary heart failure phenotyping parameter. European Journal of Heart Failure, 24(7), 1158–1161. https://doi.org/10.1002/ejhf.2576
Ma, X., Jung, C., Chang, H.-Y., Richards, T. M., & Kharrazi, H. (2020). Assessing the Population-Level Correlation of Medication Regimen Complexity and Adherence Indices Using Electronic Health Records and Insurance Claims. Journal of Managed Care & Specialty Pharmacy, 26(7), 10.18553/jmcp.2020.26.7.860. https://doi.org/10.18553/jmcp.2020.26.7.860
Mansur, N., Weiss, A., & Beloosesky, Y. (2012). Looking beyond polypharmacy: Quantification of medication regimen complexity in the elderly. The American Journal of Geriatric Pharmacotherapy, 10(4), 223–229. https://doi.org/10.1016/j.amjopharm.2012.06.002
Masoudi, F. A., & Krumholz, H. M. (2003). Polypharmacy and comorbidity in heart failure. BMJ : British Medical Journal, 327(7414), 513–514.
Mastromarino, V., Casenghi, M., Testa, M., Gabriele, E., Coluccia, R., Rubattu, S., & Volpe, M. (2014). Polypharmacy in heart failure patients. Current Heart Failure Reports, 11(2), 212–219. https://doi.org/10.1007/s11897-014-0186-8
Pantuzza, L. L., Ceccato, M. das G. B., Silveira, M. R., Junqueira, L. M. R., & Reis, A. M. M. (2017). Association between medication regimen complexity and pharmacotherapy adherence: A systematic review. European Journal of Clinical Pharmacology, 73(11), 1475–1489. https://doi.org/10.1007/s00228-017-2315-2
Percival, M., Cottrell, W. N., & Jayasinghe, R. (2012). Exploring the beliefs of heart failure patients towards their heart failure medicines and self care activities. International Journal of Clinical Pharmacy, 34(4), 618–625. https://doi.org/10.1007/s11096-012-9655-x
Phillips, L. A., Diefenbach, M., Kronish, I. M., Negron, R. M., & Horowitz, C. R. (2014). The Necessity-Concerns-Framework: A Multidimensional Theory Benefits from Multidimensional Analysis. Annals of Behavioral Medicine : A Publication of the Society of Behavioral Medicine, 48(1), 7–16. https://doi.org/10.1007/s12160-013-9579-2
Rafhi, E., Stupans, I., Stevens, J. E., Soo Park, J., & Wang, K. N. (2025). The influence of beliefs and health literacy on medication-related outcomes in older adults: A cross-sectional study. Research in Social and Administrative Pharmacy, 21(1), 47–55. https://doi.org/10.1016/j.sapharm.2024.10.003
Safwana Al-Tahesh et al. Predictors and impact of medication non-adherence in heart failure patients: a retrospective cohort from a tertiary hospital in Yemen. Pan African Medical Journal. 2026;53:9. [doi: 10.11604/pamj.2026.53.9.48712]
Savarese, G., Stolfo, D., Sinagra, G., & Lund, L. H. (2022). Heart failure with mid-range or mildly reduced ejection fraction. Nature Reviews. Cardiology, 19(2), 100–116. https://doi.org/10.1038/s41569-021-00605-5
Schoonover, H., Corbett, C. F., Weeks, D. L., Willson, M. N., & Setter, S. M. (2014). Predicting potential postdischarge adverse drug events and 30-day unplanned hospital readmissions from medication regimen complexity. Journal of Patient Safety, 10(4), 186–191. https://doi.org/10.1097/PTS.0000000000000067
Stange, D., Kriston, L., von Wolff, A., Baehr, M., & Dartsch, D. C. (2013). Medication complexity, prescription behaviour and patient adherence at the interface between ambulatory and stationary medical care. European Journal of Clinical Pharmacology, 69(3), 573–580. https://doi.org/10.1007/s00228-012-1342-2
Supramaniam, P., binti Ali, A., Li Yun, C., Pei Yi, C., binti Shaari, A., binti Kamaruzaman, N. H., Jia Yi, S., Keat Ming, T., Yuan Liang, W., & Pei Wen, Y. (2019). Reliability and validity of Beliefs on Medicine Questionnaire (BMQ) in diabetes mellitus patients: Malay Translated Version. International Journal of Scientific and Research Publications (IJSRP), 9(2), p8609. https://doi.org/10.29322/IJSRP.9.02.2019.p8609
Wei, L., Champman, S., Li, X., Li, X., Li, S., Chen, R., Bo, N., Chater, A., & Horne, R. (2017). Beliefs about medicines and non-adherence in patients with stroke, diabetes mellitus and rheumatoid arthritis: A cross-sectional study in China. BMJ Open, 7(10), e017293. https://doi.org/10.1136/bmjopen-2017-017293
Yasin, N. M., Filliana, U., & Kristina, S. A. (2024). Pengaruh Brief Counseling Apoteker terhadap Kepatuhan Pengobatan dan Perbaikan Tekanan Darah Pasien Hemodialisa. Majalah Farmaseutik, 20(3), 324. https://doi.org/10.22146/FARMASEUTIK.V20I3.92562.